Digital biomarkers, which are consumer-generated physiological and behavioral measures collected through connected digital tools, are showing great potential as powerful and cost-efficient tools to track health and predict outcomes, according to a new Rock Health report.
The report argues that digital biomarkers can extend the collection of population level health data over time and introduce longitudinal data for individual consumers. Also, they could lend a level of subjectivity — if wielded accurately — in fields like psychiatry and neurology.
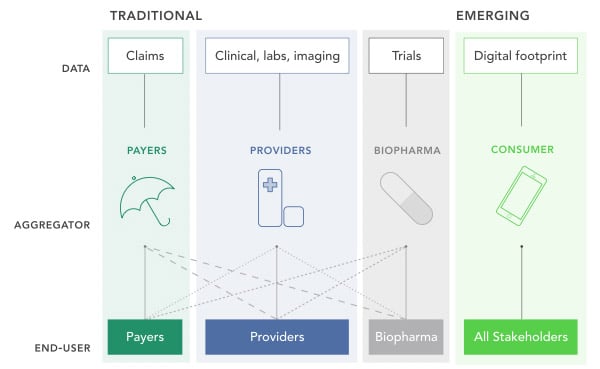
Payers could use digital biomarkers to inform insurers on the best coverage for their customers and design appropriate reimbursement policies.
We are still in the early days of this technology and there’s a lot of work ahead before it proves its worth.Providers on their end could dive into digital biomarker data to identify high-risk, high-cost individuals, and predict readmission. Digital tools could be used to monitor disease progression, and react accordingly by providing interventions in near real-time. On the other hand, these same tools could improve the objectivity of diagnoses and treatment selection.
Finally, biopharma companies could improve the quality and efficiency of clinical trials. Everything from clinical trial recruitment to disease progression monitoring could be studied more accurately and in a more cost-effective manner with the help of data generated by digital biomarkers.
However, we’re still in the early days of this technology and there’s a lot of work ahead before it proves its worth. A recent, Eric Topol-led, six-month study with several patients that had submitted insurance claims for hypertension, diabetes, or arrhythmia published in PeerJ last month, hasn’t produced desired results.
“There was little evidence of differences in health care costs or utilization as a result of the intervention,” the study concluded.
There were little to no differences between control and intervention groups, despite the steady surveillance of digital biomarkers. A bit of an improvement was noticed in terms of self-management, but by and large patients didn’t appear to benefit from the additional monitoring.
“This result suggests there are no large short-term increases or decreases in health care costs or utilization associated with monitoring chronic health conditions using mobile health or digital medicine technologies,” the paper says.
[Via: MedCityNews]